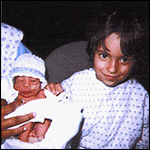
I am sitting in front of an incubator in the Newborn Intensive Care Unit of
Manatee Memorial Hospital, staring through the Plexiglas at the little boy
inside. He is all of 3 pounds, 4 ounces.
There are cartoon stickers on his chest hiding the wires spiraling out of the
incubator. The wires trail upwards to a monitor with its white lines, rolling
up and down across a black screen, like some obscene cyber roller coaster.
The baby is not an hour old. The IV bag, dangling next to the monitor, drips.
Fluid runs down a clear aquarium-like tube. It seeps through the needle
penetrating his tiny little body. A similar tube disappears down one of his
nostrils. In all my wildest dreams, I never thought the joy of having a
child could turn into such a nightmare.
It is not my first child. My wife and I have two others. Our first, born in
Brooklyn, New York, came kicking and screaming into this world at a healthy 6
pounds, 13 ounces. Our second, a boy, tipped the scale at 8 pounds, 5 ounces.
We didn't do anything different this time around and yet, this time around,
everything is different. During a routine check-up, we are told to go to the
Emergency Room. We are told the placenta has detached from the baby. The baby
isn't due for nearly two months and it has to come out, now.
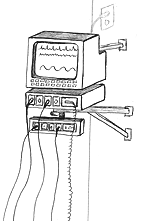 An alarm on the monitor sounds and my heart sinks into my stomach. I stare at
the screen. The baby has something called retinitis, a red flag for a virus
called CMV. They haven't confirmed this yet, but I am being presented with
the possibility of blindness, deafness, mental retardation. Yes, the virus
can be deadly to infants. I don't know if the baby is going to live or die
and then lines on the monitor are rising and falling all over again.
The doctor leaves and the nurses take over. They show me how to open the
little portal of the incubator, encouraging me to touch him. They explain
that the tube in his nose is a feeding tube. I learn about Apnea and what the
lines on the monitor represent. They introduce me to several of the other
babies and not all of them are in incubators. One isn't even hooked to a
fetal monitor anymore.
An alarm on the monitor sounds and my heart sinks into my stomach. I stare at
the screen. The baby has something called retinitis, a red flag for a virus
called CMV. They haven't confirmed this yet, but I am being presented with
the possibility of blindness, deafness, mental retardation. Yes, the virus
can be deadly to infants. I don't know if the baby is going to live or die
and then lines on the monitor are rising and falling all over again.
The doctor leaves and the nurses take over. They show me how to open the
little portal of the incubator, encouraging me to touch him. They explain
that the tube in his nose is a feeding tube. I learn about Apnea and what the
lines on the monitor represent. They introduce me to several of the other
babies and not all of them are in incubators. One isn't even hooked to a
fetal monitor anymore.
"She'll be going home tomorrow," the nurse explains. "Your baby will get
there."
I look at the nurse. It's the first positive thing I have heard all day.
Over the next few days my wife and I are encouraged to hold the baby. By
week's end bottle feeding is attempted. The boy does poorly and we have to
endure watching the plastic syringe deliver the food through the feeding
tube. We help change his diapers. Have you ever changed the diaper of a
preemie? I keep thinking of the cabbage patch dolls my daughter plays with.
I keep hearing things outside of the hospital. Friends and neighbors are
whispering about Manatee Memorial. None of it is terribly flattering. I never
thought to ask if they've ever had a baby at Manatee Memorial.
After 21 days there is concern over a heart murmur. A sonogram is taken. The
results are sent by courier to the All Children's Hospital in St. Petersburg.
The report, the following day, suggests there is no abnormal activity in the
heart.
On another visit, we are seated in front of a TV. One of the nurses feeds a
VCR into a video and we watch a film on infant CPR. When the movie ends, a
dummy is brought out and we are shown by the nurse what to do should the baby
stop breathing. After watching all of this, we are asked to get intimate with
the dummy, and yes, for a while there, one has to wonder who the real dummy
is.
Lennon Matthew was in the NIC Unit for 26 days. It was a horrible four weeks.
They give you a worst-case scenario and tell you to hope for the best, and in
the end everything did turn out all right. The retinitis cleared. There were
no traces of CMV. Further tests last week finally ruled out Toxoplasma. The
forecast is for a normal, healthy baby. He is eating well and gaining weight,
now at 5 pounds, 4 ounces. He is small, still, and the only real concern
remaining relates to bone-growth. Our pediatrician says not to worry about
it, it'll be 18 months before anyone can say whether this kid will grow to an
average height.
My mother died some ten years ago. This person that is in your life, everyday
of your life, comes home from dinner one night and collapses. She is rushed
to the Emergency Room and the next thing you know is they're uttering that C
word, cancer. They give you worst-case scenarios and tell you to hope for the
best, and you do hope for the best, 'cause you've seen those days that mom
has the flu, or a little minor surgery but in the end everything is all
right. Everyone gets well. And then one day they mention that C word, and
over the next several months you watch this human body shrivel up and blow
away. Everyone doesn't always get well anymore. You suddenly realize how
vulnerable we truly are.
 Our first baby was born in one of the finest hospitals in Brooklyn, New York.
I spent a year in Cleveland, Ohio, on a job that saw me shuttling from
hospital to hospital. The quality of care at Manatee Memorial Hospital is
second to none.
Our first baby was born in one of the finest hospitals in Brooklyn, New York.
I spent a year in Cleveland, Ohio, on a job that saw me shuttling from
hospital to hospital. The quality of care at Manatee Memorial Hospital is
second to none.
The staff of the NIC Unit proved to be as skillful in their
handling of parents as they are in their care of infants. Whether it's
comforting a crier, bathing a newborn, changing diapers, or performing
emergency care, it takes a truly special breed to work the NICU. The task at
hand is constant. At times, there isn't a moment's rest. The staff at Manatee
Memorial's NIC Unit are just such a breed. Perhaps, even, a roomful of
angels, caring for our most vulnerable of dreams.

